
Open Access
Editorial
Exploration of Asthma & Allergy, where science, evidence, and vision can improve clinical practice
Giorgio Walter Canonica, Enrico Heffler
Published: March 01, 2023 Explor Asthma Allergy. 2023;1:1–3

Open Access
Mini Review
TSLP and asthma: fellow travelers
David El-Qutob, Antonio Letran
Published: April 14, 2023 Explor Asthma Allergy. 2023;1:4–10
Open Access
Original Article
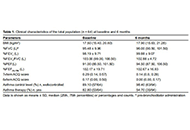
An exploratory study on the validity and reliability of the Greek translation of Juniper’s Asthma Control Questionnaire in pediatric patients in Greece
Maria M. Papamichael ... Bircan Erbas
Published: April 23, 2023 Explor Asthma Allergy. 2023;1:11–19
Open Access
Case Report
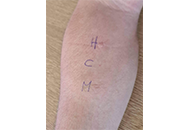
Isolated lettuce allergy in a medical student: case report and review of the literature
Kyle Alexander ... Nicolaos Nicolaou
Published: April 26, 2023 Explor Asthma Allergy. 2023;1:20–27
Open Access
Letter to the Editor
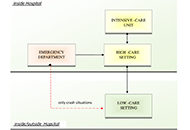
Allergists/immunologists facing the coronavirus disease 2019 pandemic: the experience of managing a low-care setting
Laura Franceschini ... Alessandro Farsi
Published: April 27, 2023 Explor Asthma Allergy. 2023;1:28–30
Open Access
Review
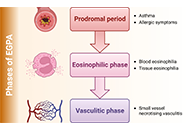
New therapeutic approaches with biological drugs for eosinophilic granulomatosis with polyangiitis
Alejandra Carrón-Herrero ... Giovanni Paoletti
Published: June 08, 2023 Explor Asthma Allergy. 2023;1:31–48
This article belongs to the special issue The Era of Biologics in Allergy
Open Access
Original Article
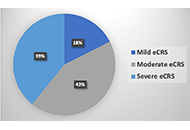
Assessing chronic rhinosinusitis with nasal polyps severity by “Japanese epidemiological survey of refractory eosinophilic chronic rhinosinusitis” algorithm
Sérgio Duarte Dortas ... Solange Oliveira Rodrigues Valle
Published: June 16, 2023 Explor Asthma Allergy. 2023;1:49–54
This article belongs to the special issue Precision Medicine in Allergy and Rhinology
Open Access
Case Report
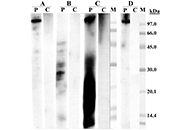
Food fish allergy as a result of occupational exposure to fish collagen
Felipe Santos Vicente ... Borja Bartolomé Zavala
Published: June 30, 2023 Explor Asthma Allergy. 2023;1:55–59

Open Access
Review
Eosinophilic gastrointestinal disorders: new perspectives and the emerging role of biological therapies
Francesca Losa, Arianna Cingolani
Published: June 30, 2023 Explor Asthma Allergy. 2023;1:60–72
This article belongs to the special issue The Era of Biologics in Allergy

Open Access
Correction
Correction: Omega-5-gliadin-specific immunoglobulin E-positive, but wheat-specific immunoglobulin E-negative wheat allergy dependent on augmentation factors—a frequent presentation
Editorial Office
Published: January 17, 2024 Explor Asthma Allergy. 2024;2:1

Open Access
Case Report
Clinical responses and relapses in omalizumab-assisted desensitization to food in children: long-term evolution in real life
Angel Mazon ... Antonio Nieto
Published: January 30, 2024 Explor Asthma Allergy. 2024;2:2–8
This article belongs to the special issue The Different Faces of Food Allergy

Open Access
Review
Management of asthma using probiotics
Amar P. Garg ... Bajeerao Patil
Published: February 20, 2024 Explor Asthma Allergy. 2024;2:9–32
This article belongs to the special issue Asthma and its Relationship with Psychological and Psychopathological Factors

Open Access
Review
Evaluation of ongoing mepolizumab treatment in chronic rhinosinusitis with nasal polyps
Ludger Klimek ... Claus Bachert
Published: February 22, 2024 Explor Asthma Allergy. 2024;2:33–48
This article belongs to the special issue Update on Chronic RhinoSinusitis

Open Access
Review
Predictive value of skin testing with excipients for COVID-19 vaccines
Fabio Viggiani ... Eustachio Nettis
Published: February 27, 2024 Explor Asthma Allergy. 2024;2:49–64
Open Access
Mini Review
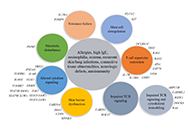
Food allergy as one of the faces of primary immunodeficiency
Polina Kostova ... Guergana Petrova
Published: February 29, 2024 Explor Asthma Allergy. 2024;2:65–75
This article belongs to the special issue The Different Faces of Food Allergy

Open Access
Mini Review
Allergen-specific immunotherapy for allergic asthma: What’s new?
Chiara Asperti ... Stephen R. Durham
Published: February 29, 2024 Explor Asthma Allergy. 2024;2:76–84
This article belongs to the special issue Precision Medicine in Allergy and Rhinology

Open Access
Original Article
Small airway disease assessed by parameters of small airway dysfunction in patients with asthma, asthma-chronic obstructive pulmonary disease-overlap, and chronic obstructive pulmonary disease
Richard Kraemer, Heinrich Matthys
Published: April 02, 2024 Explor Asthma Allergy. 2024;2:85–96
Open Access
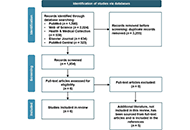
Review
Catching your breath: unraveling the intricate connection between panic disorder and asthma
Graziella Chiara Prezzavento
Published: April 08, 2024 Explor Asthma Allergy. 2024;2:97–110
This article belongs to the special issue Asthma and its Relationship with Psychological and Psychopathological Factors
Open Access
Review
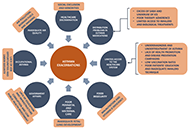
How to implement the anti-inflammatory reliever treatment proposed by the Global Initiative for Asthma in low- and middle-income countries
Carlos A. Torres-Duque ... Abraham Alí-Munive
Published: June 12, 2024 Explor Asthma Allergy. 2024;2:219–232
Open Access
Review
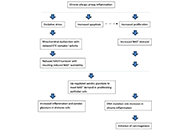
Metabolic adaption of epithelial cells in asthma: a window to the initiation of carcinogenesis?
Thomas Dymond
Published: June 12, 2024 Explor Asthma Allergy. 2024;2:233–244
This article belongs to the special issue Airway Epithelial Cells in Asthma

