Open Access
Review
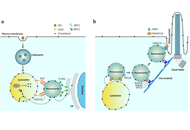
Peroxisomes in intracellular cholesterol transport: from basic physiology to brain pathology
Jian Xiao ... Jie Luo
Published: December 30, 2021 Explor Neuroprot Ther. 2021;1:127–145
This article belongs to the special issue Cholesterol Dyshomeostasis in Neurological Diseases
Open Access
Review
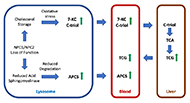
Advancing diagnosis and treatment of Niemann-Pick C disease through biomarker discovery
Xuntian Jiang, Daniel S. Ory
Published: December 30, 2021 Explor Neuroprot Ther. 2021;1:146–158
This article belongs to the special issue Cholesterol Dyshomeostasis in Neurological Diseases
Open Access
Review
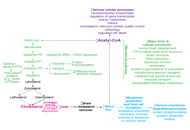
Targeting cytochrome P450 46A1 and brain cholesterol 24-hydroxylation to treat neurodegenerative diseases
Irina A. Pikuleva
Published: December 30, 2021 Explor Neuroprot Ther. 2021;1:159–172
This article belongs to the special issue Cholesterol Dyshomeostasis in Neurological Diseases
Open Access
Review
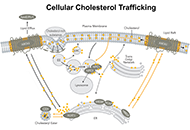
Blocking cholesterol storage to treat Alzheimer’s disease
Ta Yuan Chang ... James G. Gow
Published: December 30, 2021 Explor Neuroprot Ther. 2021;1:173–184
This article belongs to the special issue Cholesterol Dyshomeostasis in Neurological Diseases
Open Access
Review
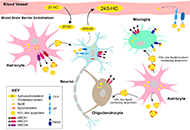
Balancing cholesterol in the brain: from synthesis to disposal
Lydia Qian ... Andrew J. Brown
Published: January 05, 2022 Explor Neuroprot Ther. 2022;2:1–27
This article belongs to the special issue Cholesterol Dyshomeostasis in Neurological Diseases
Open Access
Review
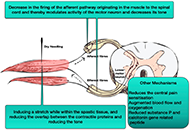
Dry needling in stroke
Nirmal Surya, Guhan Ramamurthy
Published: February 17, 2022 Explor Neuroprot Ther. 2022;2:28–35
This article belongs to the special issue Dry Needling for Neurological Disorders
Open Access
Systematic Review
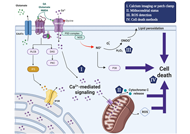
Various facets of excitotoxicity
Talita Glaser ... Henning Ulrich
Published: February 23, 2022 Explor Neuroprot Ther. 2022;2:36–64
Open Access
Review
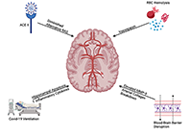
Subarachnoid hemorrhage: management considerations for COVID-19
Eric J. Panther, Brandon Lucke-Wold
Published: March 02, 2022 Explor Neuroprot Ther. 2022;2:65–73
This article belongs to the special issue Emerging Concepts in Subarachnoid Hemorrhage
Open Access
Perspective
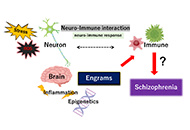
Gut microbiota could modulate the effects of neuro-immune responses and memory traces via the gut-brain-immune axis in schizophrenia
Haruka Sawamura ... Satoru Matsuda
Published: April 24, 2022 Explor Neuroprot Ther. 2022;2:74–86
This article belongs to the special issue Intervention of Neuroimmune Responses

Open Access
Review
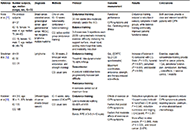
The role of physical activity against chemotherapy-induced peripheral neuropathy: a narrative review
Daniele Diotti ... Lucio Marinelli
Published: April 28, 2022 Explor Neuroprot Ther. 2022;2:87–99

Open Access
Original Article
Combined effects of dry needling and exercises therapy on muscle spasticity and motor function in chronic stroke: a pretest-posttest pilot study
Seyedeh Saeideh Babazadeh-Zavieh ... Korosh Mansoori
Published: June 20, 2022 Explor Neuroprot Ther. 2022;2:100–109
This article belongs to the special issue Dry Needling for Neurological Disorders
Open Access
Perspective
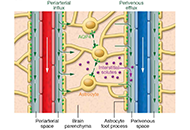
Can meditation-based approaches improve the cleansing power of the glymphatic system?
Peter Wostyn, Piet Goddaer
Published: June 20, 2022 Explor Neuroprot Ther. 2022;2:110–117
Open Access
Review
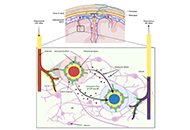
The glymphatic system and subarachnoid hemorrhage: disruption and recovery
Stephan Quintin ... Brandon Lucke-Wold
Published: June 21, 2022 Explor Neuroprot Ther. 2022;2:118–130
This article belongs to the special issue Emerging Concepts in Subarachnoid Hemorrhage

Open Access
Review
Economics of dry needling and botulinum toxin type A for treatment of post-stroke spasticity: a review
Daniel Fernández ... Eva María Gómez-Trullén
Published: June 30, 2022 Explor Neuroprot Ther. 2022;2:131–140
This article belongs to the special issue Dry Needling for Neurological Disorders

Open Access
Editorial
Science plus technology to address challenges in determining the efficacy of neuroprotective/neurorestorative therapies
Rafael Franco
Published: August 05, 2021 Explor Neuroprot Ther. 2021;1:1–6

Open Access
Letter to the Editor
P2X7 receptor involvement in COVID-19 disease
Peter Illes
Published: August 05, 2021 Explor Neuroprot Ther. 2021;1:7–9
Open Access
Review
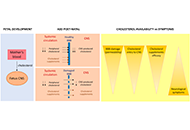
Cholesterol in autism spectrum disorders
Rafael Franco ... Irene Reyes-Resina
Published: August 05, 2021 Explor Neuroprot Ther. 2021;1:10–18
This article belongs to the special issue Cholesterol Dyshomeostasis in Neurological Diseases
Open Access
Review
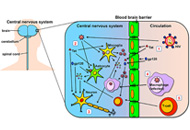
Neurological complications during HIV infection
Jose M. Martinez-Navio
Published: August 05, 2021 Explor Neuroprot Ther. 2021;1:19–32
Open Access
Review
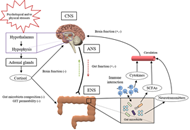
Gut microbial imbalance and neurodegenerative proteinopathies: from molecular mechanisms to prospects of clinical applications
Paula Alonso-García ... Eva Martínez-Pinilla
Published: August 05, 2021 Explor Neuroprot Ther. 2021;1:33–54
Open Access
Review
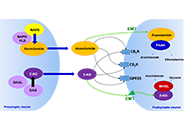
Therapeutic potential of the cannabinoid receptor 2 in neuropsychiatry
María S. García-Gutiérrez ... Jorge Manzanares
Published: August 05, 2021 Explor Neuroprot Ther. 2021;1:55–71

