
Open Access
Editorial
Cutting edges in neuroscience to exceed borders
Dirk M. Hermann
Published: September 01, 2022 Explor Neurosci. 2022;1:1–3
Open Access
Review
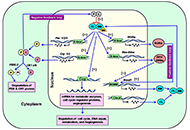
Impact of circadian clock dysfunction on human health
Saptadip Samanta, Sk Asif Ali
Published: September 29, 2022 Explor Neurosci. 2022;1:4–30
This article belongs to the special issue Circadian Rhythm and Melatonin
Open Access
Review
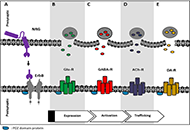
Neuregulins: subcellular localization, signaling pathways and their relationship with neuroplasticity and neurological diseases
Marines Longart ... Juan Carlos Martínez
Published: September 29, 2022 Explor Neurosci. 2022;1:31–53

Open Access
Perspective
Recent developments and future perspectives of neuropathology
Kurt A. Jellinger
Published: September 30, 2022 Explor Neurosci. 2022;1:54–60
Open Access
Review
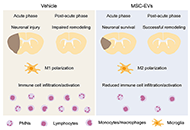
Neuroprotective and neurorestorative actions of mesenchymal stromal cell-derived small extracellular vesicles in the ischemic brain
Chen Wang ... Dirk M. Hermann
Published: October 09, 2022 Explor Neurosci. 2022;1:61–74

Open Access
Perspective
Should we rethink neurodegeneration?
Jussi O. T. Sipilä
Published: December 26, 2022 Explor Neurosci. 2022;1:75–82

Open Access
Review
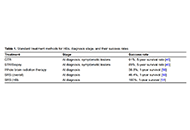
Updates in mechanical thrombectomy
Kevin Pierre ... Brandon Lucke-Wold
Published: December 30, 2022 Explor Neurosci. 2022;1:83–99
Open Access
Review
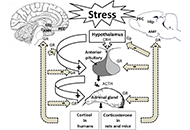
Cellular and molecular mechanisms of stress-induced memory impairment
Ameneh Rezayof ... Shiva Hashemizadeh
Published: December 30, 2022 Explor Neurosci. 2022;1:100–119
Open Access
Review
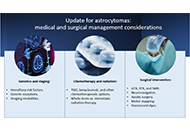
Update for astrocytomas: medical and surgical management considerations
Matthew Willman ... Brandon Lucke-Wold
Published: February 23, 2023 Explor Neurosci. 2023;2:1–26
Open Access
Systematic Review
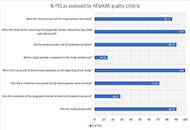
Genetic plasma biomarkers associated with ischemic stroke
Mihai Andrei Ruscu ... Aurel Popa-Wagner
Published: February 26, 2023 Explor Neurosci. 2023;2:27–47
This article belongs to the special issue Cerebral Ischemia, Genetics, Comorbidities, Risk Factors and New Therapeutic Options for Neurorestoration

Open Access
Editorial
Treatment concept successfully translated into human patients
Dirk M. Hermann
Published: February 28, 2023 Explor Neurosci. 2023;2:48–51
Open Access
Original Article
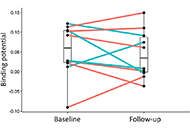
The effect of the tumour necrosis factor-alpha-inhibitor etanercept on microglial activation patients with mild cognitive impairment—a PET study
Alexander Gerhard ... Clive Holmes
Published: March 26, 2023 Explor Neurosci. 2023;2:52–66

Open Access
Review
Metabolic correction of neurodegenerative pathologies: the role of macronutrients and timing
Yuri Zilberter, Tanya Zilberter
Published: April 21, 2023 Explor Neurosci. 2023;2:67–81
Open Access
Review
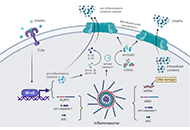
Inflammatory responses involved in post-cardiac arrest brain injury: mechanisms, regulation, and therapeutic potential
Yuzhen Zhang ... Kaibin Huang
Published: April 26, 2023 Explor Neurosci. 2023;2:82–97

Open Access
Perspective
Mesenchymal stem cell stroke therapy: current limitations in its clinical translation
Ylenia Pastorello, Mark Slevin
Published: June 28, 2023 Explor Neurosci. 2023;2:98–105

Open Access
Review
Therapeutic potential of extracellular vesicles in Parkinson’s disease
Michelli Ramires Teixeira ... Rodrigo Pinheiro Araldi
Published: June 29, 2023 Explor Neurosci. 2023;2:106–122
Open Access
Review
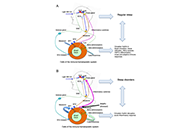
Circadian regulation of the immune-hematopoietic system
Georges Maestroni
Published: June 30, 2023 Explor Neurosci. 2023;2:123–139
This article belongs to the special issue Circadian Rhythm and Melatonin

Open Access
Review
Emerging therapies of hemangioblastomas
Chaitanya Sanghadia ... Brandon Lucke-Wold
Published: December 29, 2023 Explor Neurosci. 2023;2:318–330
This article belongs to the special issue Cerebral Ischemia, Genetics, Comorbidities, Risk Factors and New Therapeutic Options for Neurorestoration
Open Access
Review
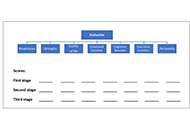
Psychology of bipolar depression: revisiting past and present researches, prospects ahead, and moving toward future directions
Behrooz Afshari
Published: December 29, 2023 Explor Neurosci. 2023;2:331–349
This article belongs to the special issue Novel Therapeutic Approaches for the Treatment of Depression

Open Access
Review
Connecting the ends: signaling via receptor tyrosine kinases and cytoskeletal degradation in neurodegeneration
Priyanka Sengupta ... Debashis Mukhopadhyay
Published: February 20, 2024 Explor Neurosci. 2024;3:1–26
This article belongs to the special issue Alzheimer’s Disease

