Decoding the impact of autoinflammatory/autoimmune diseases on inner ear harmony and hearing loss
Autoimmune and autoinflammatory diseases affecting the inner ear can cause symptoms such as hearing loss, imbalance, vertigo, and tinnitus, presenting demanding and often underdiagnosed conditions.
[...] Read more.
Autoimmune and autoinflammatory diseases affecting the inner ear can cause symptoms such as hearing loss, imbalance, vertigo, and tinnitus, presenting demanding and often underdiagnosed conditions. Diagnostic challenges arise due to their diverse manifestations, potential long-term consequences, and the absence of specific serological markers, necessitating a multidisciplinary approach combining clinical evaluation, audiological assessments, and imaging techniques. Various autoimmune disorders, including systemic lupus erythematosus, rheumatoid arthritis, and Sjogren’s syndrome, have been implicated in immune-mediated damage to auditory structures, resulting in inner ear dysfunction. Inflammatory processes in autoinflammatory diseases like Cogan’s syndrome and relapsing polychondritis can also affect the inner ear. While the exact mechanisms of inner ear involvement in these conditions are still being studied, immune-mediated inflammation, damage to auditory structures, and vascular involvement play significant roles in auditory impairments. Treatment strategies primarily focus on immunomodulation and inflammation control using corticosteroids, immunosuppressants, and targeted biologic agents to ameliorate symptoms and preserve hearing function. Hearing aids and cochlear implants may be also considered for severe hearing loss. Individualized approaches are necessary due to patient response heterogeneity. This review provides a concise overview of key autoimmune and autoinflammatory diseases impacting the inner ear, highlighting clinical manifestations, diagnostics, pathophysiology, and treatment options. Early recognition and appropriate management are crucial for optimizing patient outcomes. Further research is needed to understand underlying mechanisms and identify novel therapeutic targets. Collaboration between otolaryngologists, rheumatologists, and immunologists is crucial for improving the quality of life in these complex conditions.
Michail Athanasopoulos ... Ioannis Athanasopoulos
Autoimmune and autoinflammatory diseases affecting the inner ear can cause symptoms such as hearing loss, imbalance, vertigo, and tinnitus, presenting demanding and often underdiagnosed conditions. Diagnostic challenges arise due to their diverse manifestations, potential long-term consequences, and the absence of specific serological markers, necessitating a multidisciplinary approach combining clinical evaluation, audiological assessments, and imaging techniques. Various autoimmune disorders, including systemic lupus erythematosus, rheumatoid arthritis, and Sjogren’s syndrome, have been implicated in immune-mediated damage to auditory structures, resulting in inner ear dysfunction. Inflammatory processes in autoinflammatory diseases like Cogan’s syndrome and relapsing polychondritis can also affect the inner ear. While the exact mechanisms of inner ear involvement in these conditions are still being studied, immune-mediated inflammation, damage to auditory structures, and vascular involvement play significant roles in auditory impairments. Treatment strategies primarily focus on immunomodulation and inflammation control using corticosteroids, immunosuppressants, and targeted biologic agents to ameliorate symptoms and preserve hearing function. Hearing aids and cochlear implants may be also considered for severe hearing loss. Individualized approaches are necessary due to patient response heterogeneity. This review provides a concise overview of key autoimmune and autoinflammatory diseases impacting the inner ear, highlighting clinical manifestations, diagnostics, pathophysiology, and treatment options. Early recognition and appropriate management are crucial for optimizing patient outcomes. Further research is needed to understand underlying mechanisms and identify novel therapeutic targets. Collaboration between otolaryngologists, rheumatologists, and immunologists is crucial for improving the quality of life in these complex conditions.
 Periodontitis and lipopolysaccharides: How far have we understood?Open AccessReviewPeriodontitis is a ubiquitous chronic inflammatory worldwide disease. The multiplicity of gram-negative microbiomes and their endotoxins, such as lipopolysaccharides (LPS), play a crucial role in it [...] Read more.Spoorthi Ravi Banavar ... Suan Phaik KhooPublished: February 29, 2024 Explor Immunol. 2024;4:129–151
Periodontitis and lipopolysaccharides: How far have we understood?Open AccessReviewPeriodontitis is a ubiquitous chronic inflammatory worldwide disease. The multiplicity of gram-negative microbiomes and their endotoxins, such as lipopolysaccharides (LPS), play a crucial role in it [...] Read more.Spoorthi Ravi Banavar ... Suan Phaik KhooPublished: February 29, 2024 Explor Immunol. 2024;4:129–151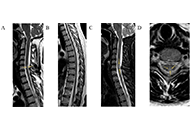 Myelitis associated with COVID-19: clinical, radiological, and laboratory characteristicsOpen AccessOriginal ArticleAim: The current study aimed to describe various types of myelitis associated with a novel coronavirus infection [coronavirus disease 2019 (COVID-19)] as well as to analyze cytokine profiles and cerebrospinal fluid (CSF) parameter [...] Read more.Aleksandra Kozlova ... Maria ZakharovaPublished: February 29, 2024 Explor Immunol. 2024;4:115–128
Myelitis associated with COVID-19: clinical, radiological, and laboratory characteristicsOpen AccessOriginal ArticleAim: The current study aimed to describe various types of myelitis associated with a novel coronavirus infection [coronavirus disease 2019 (COVID-19)] as well as to analyze cytokine profiles and cerebrospinal fluid (CSF) parameter [...] Read more.Aleksandra Kozlova ... Maria ZakharovaPublished: February 29, 2024 Explor Immunol. 2024;4:115–128 Immune cell dynamics in male reproductive health: orchestrating immune privilege and inflammatory responsesOpen AccessMini ReviewEpididymitis or epididymo-orchitis is a common urological condition in males characterized by scrotal pain, swelling, and potential urinary symptoms. Although antibiotics can eliminate the causative [...] Read more.Yiming Zhang ... Ming WangPublished: February 28, 2024 Explor Immunol. 2024;4:106–114
Immune cell dynamics in male reproductive health: orchestrating immune privilege and inflammatory responsesOpen AccessMini ReviewEpididymitis or epididymo-orchitis is a common urological condition in males characterized by scrotal pain, swelling, and potential urinary symptoms. Although antibiotics can eliminate the causative [...] Read more.Yiming Zhang ... Ming WangPublished: February 28, 2024 Explor Immunol. 2024;4:106–114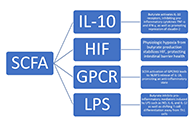 Nutritional effects on mucosal integrity and immune functionOpen AccessReviewThe intestinal mucosal barrier plays a critical role in maintaining the integrity of the gastrointestinal (GI) tract and protecting the body from harmful toxins and pathogens. Nutrition additionally [...] Read more.Lindsey B. Cundra ... David A. JohnsonPublished: February 28, 2024 Explor Immunol. 2024;4:90–105
Nutritional effects on mucosal integrity and immune functionOpen AccessReviewThe intestinal mucosal barrier plays a critical role in maintaining the integrity of the gastrointestinal (GI) tract and protecting the body from harmful toxins and pathogens. Nutrition additionally [...] Read more.Lindsey B. Cundra ... David A. JohnsonPublished: February 28, 2024 Explor Immunol. 2024;4:90–105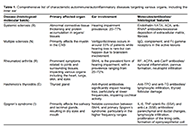 Decoding the impact of autoinflammatory/autoimmune diseases on inner ear harmony and hearing lossOpen AccessReviewAutoimmune and autoinflammatory diseases affecting the inner ear can cause symptoms such as hearing loss, imbalance, vertigo, and tinnitus, presenting demanding and often underdiagnosed conditions. [...] Read more.Michail Athanasopoulos ... Ioannis AthanasopoulosPublished: February 22, 2024 Explor Immunol. 2024;4:73–89
Decoding the impact of autoinflammatory/autoimmune diseases on inner ear harmony and hearing lossOpen AccessReviewAutoimmune and autoinflammatory diseases affecting the inner ear can cause symptoms such as hearing loss, imbalance, vertigo, and tinnitus, presenting demanding and often underdiagnosed conditions. [...] Read more.Michail Athanasopoulos ... Ioannis AthanasopoulosPublished: February 22, 2024 Explor Immunol. 2024;4:73–89 The mammary gland is intolerant to bacterial intrusionOpen AccessReviewMammals depend on the secretion of milk to rear their offspring, which exposes the organ in charge of the function, the mammary gland (MG), to bacterial threat. The essential driving force that cond [...] Read more.Pascal RainardPublished: February 06, 2024 Explor Immunol. 2024;4:59–72
The mammary gland is intolerant to bacterial intrusionOpen AccessReviewMammals depend on the secretion of milk to rear their offspring, which exposes the organ in charge of the function, the mammary gland (MG), to bacterial threat. The essential driving force that cond [...] Read more.Pascal RainardPublished: February 06, 2024 Explor Immunol. 2024;4:59–72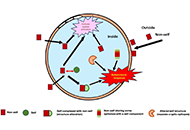 Generation and pathogenicity of autoantibodies associated to thrombosis and hemostasisOpen AccessReviewMany acquired bleeding and thrombotic complications are provoked by autoantibodies to blood coagulation factors, or to hemostasis inhibitors and regulatory proteins. If occurrence of those antibodie [...] Read more.Jean AmiralPublished: February 05, 2024 Explor Immunol. 2024;4:34–58
Generation and pathogenicity of autoantibodies associated to thrombosis and hemostasisOpen AccessReviewMany acquired bleeding and thrombotic complications are provoked by autoantibodies to blood coagulation factors, or to hemostasis inhibitors and regulatory proteins. If occurrence of those antibodie [...] Read more.Jean AmiralPublished: February 05, 2024 Explor Immunol. 2024;4:34–58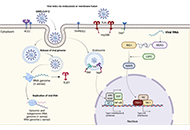 Paradigm of immune dysregulation in coronavirus disease-2019 infectionOpen AccessReviewThe coronavirus disease 2019 (COVID-19) pandemic cost 7–8 million deaths worldwide, creating an unprecedented health and economic crisis. Affecting 700 million people globally, the magnitude of th [...] Read more.Om Saswat Sahoo ... Subhradip KarmakarPublished: January 31, 2024 Explor Immunol. 2024;4:1–33
Paradigm of immune dysregulation in coronavirus disease-2019 infectionOpen AccessReviewThe coronavirus disease 2019 (COVID-19) pandemic cost 7–8 million deaths worldwide, creating an unprecedented health and economic crisis. Affecting 700 million people globally, the magnitude of th [...] Read more.Om Saswat Sahoo ... Subhradip KarmakarPublished: January 31, 2024 Explor Immunol. 2024;4:1–33