-
100 results in Exploration of Neuroprotective TherapySort byMost Cited
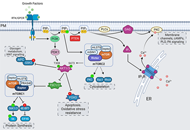 Striking a balance: PIP2 and PIP3 signaling in neuronal health and diseaseOpen AccessReviewPhosphoinositides are membrane phospholipids involved in a variety of cellular processes like growth, development, metabolism, and transport. This review focuses on the maintenance of cellular homeo [...] Read more.Kamran Tariq, Bryan W. LuikartPublished: October 29, 2021 Explor Neuroprot Ther. 2021;1:86–110
Striking a balance: PIP2 and PIP3 signaling in neuronal health and diseaseOpen AccessReviewPhosphoinositides are membrane phospholipids involved in a variety of cellular processes like growth, development, metabolism, and transport. This review focuses on the maintenance of cellular homeo [...] Read more.Kamran Tariq, Bryan W. LuikartPublished: October 29, 2021 Explor Neuroprot Ther. 2021;1:86–110
DOI: https://doi.org/10.37349/ent.2021.00008
This article belongs to the special issue Cholesterol Dyshomeostasis in Neurological Diseases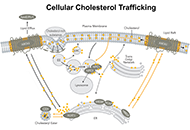 Blocking cholesterol storage to treat Alzheimer’s diseaseOpen AccessReviewCholesterol serves as an essential lipid molecule in various membrane organelles of mammalian cells. The metabolites of cholesterol also play important functions. Acyl-coenzyme A: cholesterol acyltr [...] Read more.Ta Yuan Chang ... James G. GowPublished: December 30, 2021 Explor Neuroprot Ther. 2021;1:173–184
Blocking cholesterol storage to treat Alzheimer’s diseaseOpen AccessReviewCholesterol serves as an essential lipid molecule in various membrane organelles of mammalian cells. The metabolites of cholesterol also play important functions. Acyl-coenzyme A: cholesterol acyltr [...] Read more.Ta Yuan Chang ... James G. GowPublished: December 30, 2021 Explor Neuroprot Ther. 2021;1:173–184
DOI: https://doi.org/10.37349/ent.2021.00014
This article belongs to the special issue Cholesterol Dyshomeostasis in Neurological Diseases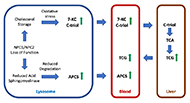 Advancing diagnosis and treatment of Niemann-Pick C disease through biomarker discoveryOpen AccessReviewNiemann-Pick C disease is a rare neurodegenerative, lysosomal storage disease caused by accumulation of unesterified cholesterol. Diagnosis of the disease is often delayed due to its rarity, the het [...] Read more.Xuntian Jiang, Daniel S. OryPublished: December 30, 2021 Explor Neuroprot Ther. 2021;1:146–158
Advancing diagnosis and treatment of Niemann-Pick C disease through biomarker discoveryOpen AccessReviewNiemann-Pick C disease is a rare neurodegenerative, lysosomal storage disease caused by accumulation of unesterified cholesterol. Diagnosis of the disease is often delayed due to its rarity, the het [...] Read more.Xuntian Jiang, Daniel S. OryPublished: December 30, 2021 Explor Neuroprot Ther. 2021;1:146–158
DOI: https://doi.org/10.37349/ent.2021.00012
This article belongs to the special issue Cholesterol Dyshomeostasis in Neurological Diseases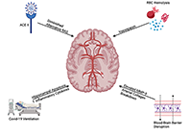 Subarachnoid hemorrhage: management considerations for COVID-19Open AccessReviewSubarachnoid hemorrhage (SAH) has deleterious outcomes for patients, and during the hospital stay, patients are susceptible to vasospasm and delayed cerebral ischemia. Coronavirus disease 2019 (COVI [...] Read more.Eric J. Panther, Brandon Lucke-WoldPublished: March 02, 2022 Explor Neuroprot Ther. 2022;2:65–73
Subarachnoid hemorrhage: management considerations for COVID-19Open AccessReviewSubarachnoid hemorrhage (SAH) has deleterious outcomes for patients, and during the hospital stay, patients are susceptible to vasospasm and delayed cerebral ischemia. Coronavirus disease 2019 (COVI [...] Read more.Eric J. Panther, Brandon Lucke-WoldPublished: March 02, 2022 Explor Neuroprot Ther. 2022;2:65–73
DOI: https://doi.org/10.37349/ent.2022.00018
This article belongs to the special issue Emerging Concepts in Subarachnoid Hemorrhage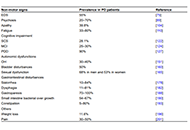 Pathophysiology of non-motor signs in Parkinson’s disease: some recent updating with brief presentationOpen AccessReviewParkinson’s disease (PD) is a progressive neurodegenerative disorder affecting 1% of the population above sixty years. It is caused by an interaction between genetic and envi [...] Read more.Khaled Radad ... Wolf-Dieter RauschPublished: February 27, 2023 Explor Neuroprot Ther. 2023;3:24–46
Pathophysiology of non-motor signs in Parkinson’s disease: some recent updating with brief presentationOpen AccessReviewParkinson’s disease (PD) is a progressive neurodegenerative disorder affecting 1% of the population above sixty years. It is caused by an interaction between genetic and envi [...] Read more.Khaled Radad ... Wolf-Dieter RauschPublished: February 27, 2023 Explor Neuroprot Ther. 2023;3:24–46
DOI: https://doi.org/10.37349/ent.2023.00036
This article belongs to the special issue Parkinsons Disease: Principal Targets and Interventional Mechanisms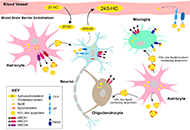 Balancing cholesterol in the brain: from synthesis to disposalOpen AccessReviewThe cholesterol is a vital component of cell membranes and myelin sheaths, and a precursor for essential molecules such as steroid hormones. In humans, cholesterol is partially obtained through the [...] Read more.Lydia Qian ... Andrew J. BrownPublished: January 05, 2022 Explor Neuroprot Ther. 2022;2:1–27
Balancing cholesterol in the brain: from synthesis to disposalOpen AccessReviewThe cholesterol is a vital component of cell membranes and myelin sheaths, and a precursor for essential molecules such as steroid hormones. In humans, cholesterol is partially obtained through the [...] Read more.Lydia Qian ... Andrew J. BrownPublished: January 05, 2022 Explor Neuroprot Ther. 2022;2:1–27
DOI: https://doi.org/10.37349/ent.2022.00015
This article belongs to the special issue Cholesterol Dyshomeostasis in Neurological Diseases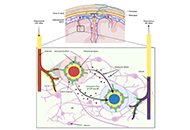 The glymphatic system and subarachnoid hemorrhage: disruption and recoveryOpen AccessReviewThe glymphatic system, or glial-lymphatic system, is a waste clearance system composed of perivascular channels formed by astrocytes that mediate the clearance of proteins and metabolites from the b [...] Read more.Stephan Quintin ... Brandon Lucke-WoldPublished: June 21, 2022 Explor Neuroprot Ther. 2022;2:118–130
The glymphatic system and subarachnoid hemorrhage: disruption and recoveryOpen AccessReviewThe glymphatic system, or glial-lymphatic system, is a waste clearance system composed of perivascular channels formed by astrocytes that mediate the clearance of proteins and metabolites from the b [...] Read more.Stephan Quintin ... Brandon Lucke-WoldPublished: June 21, 2022 Explor Neuroprot Ther. 2022;2:118–130
DOI: https://doi.org/10.37349/ent.2022.00023
This article belongs to the special issue Emerging Concepts in Subarachnoid Hemorrhage Economics of dry needling and botulinum toxin type A for treatment of post-stroke spasticity: a reviewOpen AccessReviewStroke is one of the most common causes of disability and exerts a high burden of direct and indirect costs. Stroke may cause spasticity, which limits patients’ abilities and affects the [...] Read more.Daniel Fernández ... Eva María Gómez-TrullénPublished: June 30, 2022 Explor Neuroprot Ther. 2022;2:131–140
Economics of dry needling and botulinum toxin type A for treatment of post-stroke spasticity: a reviewOpen AccessReviewStroke is one of the most common causes of disability and exerts a high burden of direct and indirect costs. Stroke may cause spasticity, which limits patients’ abilities and affects the [...] Read more.Daniel Fernández ... Eva María Gómez-TrullénPublished: June 30, 2022 Explor Neuroprot Ther. 2022;2:131–140
DOI: https://doi.org/10.37349/ent.2022.00024
This article belongs to the special issue Dry Needling for Neurological Disorders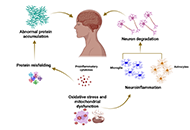 Biomarkers in neurodegenerative diseases: a broad overviewOpen AccessReviewDegeneration and dysfunction of neurons in the brain are hallmarks of neurodegenerative diseases. Over the past decades, significant efforts have been devoted to the development and validation of bi [...] Read more.Sathish Selvam, Velpandi AyyavooPublished: April 16, 2024 Explor Neuroprot Ther. 2024;4:119–147
Biomarkers in neurodegenerative diseases: a broad overviewOpen AccessReviewDegeneration and dysfunction of neurons in the brain are hallmarks of neurodegenerative diseases. Over the past decades, significant efforts have been devoted to the development and validation of bi [...] Read more.Sathish Selvam, Velpandi AyyavooPublished: April 16, 2024 Explor Neuroprot Ther. 2024;4:119–147
DOI: https://doi.org/10.37349/ent.2024.00075
This article belongs to the special issue The Future of Biomarkers in CNS Diseases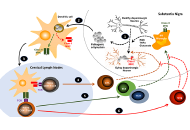 T-cell based immunotherapies for Parkinson’s diseaseOpen AccessReviewCurrent evidence indicates that neurodegeneration of dopaminergic neurons of the substantia nigra associated to Parkinson's disease is a consequence of a neuroinflammatory process in whic [...] Read more.Rodrigo PachecoPublished: October 29, 2021 Explor Neuroprot Ther. 2021;1:72–85
T-cell based immunotherapies for Parkinson’s diseaseOpen AccessReviewCurrent evidence indicates that neurodegeneration of dopaminergic neurons of the substantia nigra associated to Parkinson's disease is a consequence of a neuroinflammatory process in whic [...] Read more.Rodrigo PachecoPublished: October 29, 2021 Explor Neuroprot Ther. 2021;1:72–85
DOI: https://doi.org/10.37349/ent.2021.00007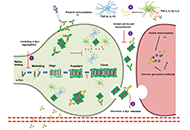 Targeting α-synuclein aggregation with immunotherapy: a promising therapeutic approach for Parkinson’s diseaseOpen AccessReviewParkinson’s disease (PD) is a prevalent neurodegenerative disease (NDD) affecting millions of individuals. The pathogenesis of PD centers around α-synuclein (α-Syn), a pivotal protein whose aggr [...] Read more.Gabriela Henriquez, Mahesh NarayanPublished: August 25, 2023 Explor Neuroprot Ther. 2023;3:207–234
Targeting α-synuclein aggregation with immunotherapy: a promising therapeutic approach for Parkinson’s diseaseOpen AccessReviewParkinson’s disease (PD) is a prevalent neurodegenerative disease (NDD) affecting millions of individuals. The pathogenesis of PD centers around α-synuclein (α-Syn), a pivotal protein whose aggr [...] Read more.Gabriela Henriquez, Mahesh NarayanPublished: August 25, 2023 Explor Neuroprot Ther. 2023;3:207–234
DOI: https://doi.org/10.37349/ent.2023.00048
This article belongs to the special issue Parkinsons Disease: Principal Targets and Interventional Mechanisms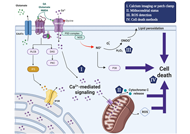 Various facets of excitotoxicityOpen AccessSystematic ReviewAim: Excitotoxicity results from unusually increased activation of excitatory amino acid receptors leading to neuronal death. Since glutamate is the main excitatory neurotransmitter in the centra [...] Read more.Talita Glaser ... Henning UlrichPublished: February 23, 2022 Explor Neuroprot Ther. 2022;2:36–64
Various facets of excitotoxicityOpen AccessSystematic ReviewAim: Excitotoxicity results from unusually increased activation of excitatory amino acid receptors leading to neuronal death. Since glutamate is the main excitatory neurotransmitter in the centra [...] Read more.Talita Glaser ... Henning UlrichPublished: February 23, 2022 Explor Neuroprot Ther. 2022;2:36–64
DOI: https://doi.org/10.37349/ent.2022.00017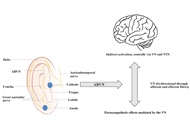 Exploration of transcutaneous vagus nerve stimulation as a treatment option for adjuvant cancer and heart failure therapyOpen AccessReviewVagus nerve stimulation (VNS) has gained prominence in the treatment of various clinical disorders such as migraine, depression, and tinnitus. Based on increased scientific knowledge of the VNS and [...] Read more.Niklas Frank ... Carola Y. FörsterPublished: October 31, 2023 Explor Neuroprot Ther. 2023;3:363–397
Exploration of transcutaneous vagus nerve stimulation as a treatment option for adjuvant cancer and heart failure therapyOpen AccessReviewVagus nerve stimulation (VNS) has gained prominence in the treatment of various clinical disorders such as migraine, depression, and tinnitus. Based on increased scientific knowledge of the VNS and [...] Read more.Niklas Frank ... Carola Y. FörsterPublished: October 31, 2023 Explor Neuroprot Ther. 2023;3:363–397
DOI: https://doi.org/10.37349/ent.2023.00056
This article belongs to the special issue Intervention of Neuroimmune Responses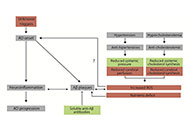 Can chronic therapeutic drug use by the elderly affect Alzheimer’s disease risk and rate of progression?Open AccessReviewThere is no approved drug capable of halting the progression of the most prevalent neurodegenerative disorders, namely Alzheimer's disease (AD) and Parkinson's disease (PD). [...] Read more.Rafael Franco, Joan Serrano-MarínPublished: February 27, 2023 Explor Neuroprot Ther 2023;3:8–23
Can chronic therapeutic drug use by the elderly affect Alzheimer’s disease risk and rate of progression?Open AccessReviewThere is no approved drug capable of halting the progression of the most prevalent neurodegenerative disorders, namely Alzheimer's disease (AD) and Parkinson's disease (PD). [...] Read more.Rafael Franco, Joan Serrano-MarínPublished: February 27, 2023 Explor Neuroprot Ther 2023;3:8–23
DOI: https://doi.org/10.37349/ent.2023.00035
This article belongs to the special issue The Urgent Need for New Hypotheses to Develop Effective Therapeutic Tools Against Alzheimers Disease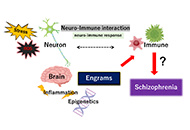 Gut microbiota could modulate the effects of neuro-immune responses and memory traces via the gut-brain-immune axis in schizophreniaOpen AccessPerspectiveAltered immunity may have destructive consequences for the integrated central nervous system. This immune response often affects progressive neurodegenerative diseases such as Parkinson’s disease and/or psychiatric disorders suc [...] Read more.Haruka Sawamura ... Satoru MatsudaPublished: April 24, 2022 Explor Neuroprot Ther. 2022;2:74–86
Gut microbiota could modulate the effects of neuro-immune responses and memory traces via the gut-brain-immune axis in schizophreniaOpen AccessPerspectiveAltered immunity may have destructive consequences for the integrated central nervous system. This immune response often affects progressive neurodegenerative diseases such as Parkinson’s disease and/or psychiatric disorders suc [...] Read more.Haruka Sawamura ... Satoru MatsudaPublished: April 24, 2022 Explor Neuroprot Ther. 2022;2:74–86
DOI: https://doi.org/10.37349/ent.2022.00019
This article belongs to the special issue Intervention of Neuroimmune Responses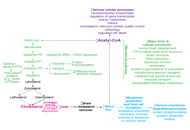 Targeting cytochrome P450 46A1 and brain cholesterol 24-hydroxylation to treat neurodegenerative diseasesOpen AccessReviewThe brain cholesterol content is determined by the balance between the pathways of in situ biosynthesis and cholesterol elimination via 24-hydroxylation catalyzed by cytochrome P450 46A1 (CYP46A1). [...] Read more.Irina A. PikulevaPublished: December 30, 2021 Explor Neuroprot Ther. 2021;1:159–172
Targeting cytochrome P450 46A1 and brain cholesterol 24-hydroxylation to treat neurodegenerative diseasesOpen AccessReviewThe brain cholesterol content is determined by the balance between the pathways of in situ biosynthesis and cholesterol elimination via 24-hydroxylation catalyzed by cytochrome P450 46A1 (CYP46A1). [...] Read more.Irina A. PikulevaPublished: December 30, 2021 Explor Neuroprot Ther. 2021;1:159–172
DOI: https://doi.org/10.37349/ent.2021.00013
This article belongs to the special issue Cholesterol Dyshomeostasis in Neurological Diseases Combined effects of dry needling and exercises therapy on muscle spasticity and motor function in chronic stroke: a pretest-posttest pilot studyOpen AccessOriginal ArticleAim: Spasticity is one of the most common symptoms in post-stroke patients. Dry needling (DN) is a relatively new method for the management of muscle spasticity. A multimodal treatment may be mor [...] Read more.Seyedeh Saeideh Babazadeh-Zavieh ... Korosh MansooriPublished: June 20, 2022 Explor Neuroprot Ther. 2022;2:100–109
Combined effects of dry needling and exercises therapy on muscle spasticity and motor function in chronic stroke: a pretest-posttest pilot studyOpen AccessOriginal ArticleAim: Spasticity is one of the most common symptoms in post-stroke patients. Dry needling (DN) is a relatively new method for the management of muscle spasticity. A multimodal treatment may be mor [...] Read more.Seyedeh Saeideh Babazadeh-Zavieh ... Korosh MansooriPublished: June 20, 2022 Explor Neuroprot Ther. 2022;2:100–109
DOI: https://doi.org/10.37349/ent.2022.00021
This article belongs to the special issue Dry Needling for Neurological Disorders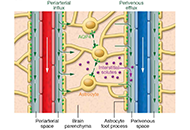 Can meditation-based approaches improve the cleansing power of the glymphatic system?Open AccessPerspectiveThe glymphatic system, first described in 2012, is a brain-wide perivascular network that plays an important role in promoting interstitial metabolic waste removal from the brain. Glymphatic pathway [...] Read more.Peter Wostyn, Piet GoddaerPublished: June 20, 2022 Explor Neuroprot Ther. 2022;2:110–117
Can meditation-based approaches improve the cleansing power of the glymphatic system?Open AccessPerspectiveThe glymphatic system, first described in 2012, is a brain-wide perivascular network that plays an important role in promoting interstitial metabolic waste removal from the brain. Glymphatic pathway [...] Read more.Peter Wostyn, Piet GoddaerPublished: June 20, 2022 Explor Neuroprot Ther. 2022;2:110–117
DOI: https://doi.org/10.37349/ent.2022.00022 Neuroprotective astroglial response to neural damage and its relevance to affective disordersOpen AccessReviewAstrocytes not only support neuronal function with essential roles in synaptic neurotransmission, action potential propagation, metabolic support, or neuroplastic and developmental adaptations. They [...] Read more.José Javier Miguel-HidalgoPublished: October 31, 2023 Explor Neuroprot Ther. 2023;3:328–345
Neuroprotective astroglial response to neural damage and its relevance to affective disordersOpen AccessReviewAstrocytes not only support neuronal function with essential roles in synaptic neurotransmission, action potential propagation, metabolic support, or neuroplastic and developmental adaptations. They [...] Read more.José Javier Miguel-HidalgoPublished: October 31, 2023 Explor Neuroprot Ther. 2023;3:328–345
DOI: https://doi.org/10.37349/ent.2023.00054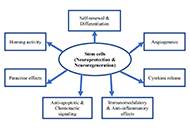 Stem cell therapy in neurological disorders: promises and concernsOpen AccessReviewSelf-neuronal regeneration is often limited or nonexistent after neuronal cell damage, making new technologies necessary for treating neurological damage. Although the brain can partially compensate [...] Read more.Said Hachimi-IdrissiPublished: October 31, 2023 Explor Neuroprot Ther. 2023;3:346–362
Stem cell therapy in neurological disorders: promises and concernsOpen AccessReviewSelf-neuronal regeneration is often limited or nonexistent after neuronal cell damage, making new technologies necessary for treating neurological damage. Although the brain can partially compensate [...] Read more.Said Hachimi-IdrissiPublished: October 31, 2023 Explor Neuroprot Ther. 2023;3:346–362
DOI: https://doi.org/10.37349/ent.2023.00055
This article belongs to the special issue Therapeutic Targets for Neuroprotection in Ischemic Stroke -
